 Monday’s Wall Street Journal featured an article entitled “What the Doctor Missed: Using Malpractice Claims to Help Physicians Avoid Diagnostic Mistakes, Delays.”
Monday’s Wall Street Journal featured an article entitled “What the Doctor Missed: Using Malpractice Claims to Help Physicians Avoid Diagnostic Mistakes, Delays.”
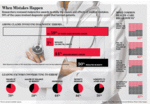
As the title suggests, medical malpractice claims are increasingly being studied by doctors and their medical malpractice insurers to avoid repeat mistakes. The knowledge that doctors gain by studying medical malpractice claims is being found to be especially important in failure-to-diagnose and misdiagnosis cases, cases which account for forty percent of all medical malpractice claims.
I’ve blogged a lot about how claims that medical malpractice lawsuits drive up health care costs ignore many offsetting gains, such as increases in patient safety that are driven by the work of medical malpractice lawyers. Increasingly, doctors themselves are acknowledging that we can run our health care system more efficiently by admitting and studying mistakes.
Monthly Archives: September 2010
Massachusetts Homeowners May Be Held Liable For Injuries Caused By Backyard Softball Game
 Massachusetts homeowners may be liable for injuries to their guests caused by sports equipment that they provide other of their guests, according to a ruling issued by the Appeals Court last week. In Judge v. Carrai, the Massachusetts Appeals Court ruled that a lawsuit can proceed against party host/homeowners for injuries that were sustained when one of their guests was hit in the back of her head by a softball hit by a teenaged guest.
Massachusetts homeowners may be liable for injuries to their guests caused by sports equipment that they provide other of their guests, according to a ruling issued by the Appeals Court last week. In Judge v. Carrai, the Massachusetts Appeals Court ruled that a lawsuit can proceed against party host/homeowners for injuries that were sustained when one of their guests was hit in the back of her head by a softball hit by a teenaged guest.
In the case, the homeowners permitted some teens and one adult to play softball with aluminum bats in the cramped confines of their small backyard. All of the equipment that was used belonged to the homeowners. At some point in the game, a very hard foul ball was hit against the house that nearly broke a skylight. The players continued on with their game and subsequently a foul ball hit Maria Judge in the back of her head while she was sitting on the homeowners’ back porch approximately 15-20 feet away from the game.
The trial court granted the Defendants’ motion for summary judgment, saying that the homeowners owed no legal duty to protect their guest from the batted ball, even after it became clear from the first foul ball, that the game posed a risk to guests on the porch. The Appeals Court disagreed and reversed the trial court.
If the guest had actually been playing in the softball game, this would have been a simple case where the guest would have been thought to have assumed the risk of injuries arising from the softball game. But because the guest was simply a bystander to the softball action, the Appeals Court had to clarify some principles of premises liability.
The Court noted that, as a general matter, “an owner or possessor of land owes to all persons lawfully on the premises a common law duty of reasonable care to maintain the property in a reasonably safe condition.” But, generally speaking, a land owner’s duty of reasonable care means a duty to protect guests from dangers in the property and not injuries caused by third parties (such as other guests on the property). In order for a land owner to be held liable to a guest for injuries caused by a third party, there must be some special legal relationship between the land owner and the guest and Massachusetts courts have normally not recognized being a social guest as forming such a special relationship. Thus, Massachusetts courts have declined to hold homeowners liable for injuries caused to their guests by other guests who bring alcohol or fireworks to a party.
But the Appeals Court found those other cases relating to fireworks and alcohol brought on the premises to be distinguishable from the case before it because, in this case, the homeowners themselves furnished the aluminum bats, balls and gloves. Thus they found it more analogous to cases where the homeowners themselves furnished alcohol or cases against the Red Sox brought by spectators injured by foul balls.
I think the Appeals Court reached the right result here but, despite the favorable ruling for the plaintiff, she will still have an uphill climb before a jury. If a jury concludes that the guest was more than 50 percent at fault – either for keeping her back turned to the softball action or for continuing to remain seated on the porch after the first foul ball – she will recover nothing. Whatever the outcome, I’m sure the homeowners will be investing in a $4.99 Wiffle Ball Bat and Ball set.
Link Roundup
- “The Easy Case For Products Liability Law,” a Harvard Law Review article by Professors Goldberg and Zipursky, defending products liability law.
- Professor Alberto Bernabe reports on the $21 million verdict that a New Hampshire jury returned against a pharmaceutical company. The plaintiff in the case developed Stevens-Johnson Syndrome from her use of a generic nonsteroidal antiinflammatory, leaving her with burns all over her body. If you are brave and not easily nauseated, you can read more about the ravages of Stevens-Johnson Syndrome here.
- This goes back aways, but Ted Frank at Point of Law blogs about the growing number of inadequate security lawsuits against banks brought by ATM customers robbed after withdrawing money.
- Eric Turkewitz on why the insurance companies aren’t like you or me.
The Judge, Medical Malpractice and Tort Reform
 A recent story out of Florida illustrates neatly what tort reform means for the victims of medical malpractice and should help most people figure out what side of the debate they come down on.
A recent story out of Florida illustrates neatly what tort reform means for the victims of medical malpractice and should help most people figure out what side of the debate they come down on.
Judge Nelson Bailey checked into a Florida hospital for a procedure to treat his diverticulitis. He checked out with a one square foot surgical sponge that surgeons forgot in his intestines. It’s one of the most common medical malpractice scenarios, one that affects 3,000 patients a year: a surgical team leaves a sponge or instrument inside a patient, who is sewn up and sent home.
The sponge of course caused an infection and abdominal pains that led Judge Bailey to go back to the doctor’s. Despite the fact that the surgical sponge was equipped with a tag that is designed to make it stand out clearly during medical imagine procedures, the sponge was not spotted over the course of several CT scans that were performed on Judge Bailey to diagnose his new abdominal pain.
By the time the radiologists caught the sponge, the infection had rotted away part of his intestine, which had to be removed. Judge Bailey can no longer venture far from a bathroom for an extended period of time and has had to give up one of his favorite hobbies: horseback riding.
One of the tort reform movement’s hobbyhorses is caps on pain and suffering damages. A number of states have adopted $250,000 caps on pain and suffering damages in medical malpractice cases. Florida has adopted a set of slightly higher caps.
Look at how those caps would apply in Judge Bailey’s cases. Bailey’s economic damages from the medical malpractice are likely to be low since he’ll continue to sit on the bench, though doubtless juries will wonder why he keeps taking breaks in the middle of trials. His future medical expenses will be next to nothing because Judge Bailey isn’t going to require long-term treatment; it’s basically as good as it gets for Judge Bailey at this point.
But for the rest of his life, Judge Bailey will be unable to carry on his favorite hobby, unable to go on long drives or hikes and, while on the bench doing his job, will probably be distracted by the rumblings of his stomach as lawyers drone on in front of him. And for that, a number of states would say he’s entitled at most to $250,000.
Good luck finding a medical malpractice lawyer to take on that case.
Judge Bailey wants the hospital that he was at to adopt new technology that would help catch surgical sponges left inside of patients. Would Good Samaritan Hospital be more likely to invest in new technology under a regime where its liability for pain and suffering is capped at $250,000 or where a jury determines its limits?
Post Script: Thanks to Professor Alberto Bernabe, who drew my attention to the comments section of The Wall Street Journal article. It was surprising how many people (even in this obviously self-selecting and non-representative group) seem to believe that caveat emptor should apply to consumers of medical services.
Checklists and Other Medical Error Reforms
 This month’s Reader’s Digest features an article entitled “Doctors Confess Their Fatal Mistakes,” which contains the stories of five haunting medical errors, only one of which resulted in any legal consequences for the practitioner (a pharmacist).
This month’s Reader’s Digest features an article entitled “Doctors Confess Their Fatal Mistakes,” which contains the stories of five haunting medical errors, only one of which resulted in any legal consequences for the practitioner (a pharmacist).
From my perspective, the most interesting story involved Dr. Peter Pronovost, an outstanding Johns Hopkins physician and MacArthur “genius grant” recipient for his work on developing checklists for doctors to follow. Dr. Provonost’s account of a medical error that he committed as a medical resident highlights two important medical reforms that could easily be undertaken to reduce the incidence of medical malpractice: implementing checklists and making sure residents are not overtired.
Dr. Pronovost, one of the leading clinical figures of his generation, helped develop medical checklists that, in a worldwide pilot study, reduced surgical deaths by 47 percent and serious complications by 36 percent. As a young resident doing specialty training in critical care, Dr. Pronovost (fatigued by not having slept within the past 24 hours) made the hasty decision to remove a patient’s breathing tube and transfer him out of ICU.
The patient’s breathing sped up and Dr. Pronovost had difficulties reintubating the patient. While Dr. Pronovost attempted to reintubate the patient, the patient was without oxygen for three to five minutes, a time period that can result in brain damage. Fortunately, Dr. Pronovost’s patient did not suffer any brain damage and did not sue for medical malpractice.
Dr. Pronovost believes that before he pulled his patient’s breathing tube he should have had to complete a medical checklist that would have revealed to him that the particular patient that he was dealing with would be difficult to reintubate. Provonost notes that NASCAR crews and airline pilots use checklists to save lives and so should doctors. Why is American medicine so resistant to checklists? Dr. Provonost thinks it has to do with the “myth that doctors are perfect.”
Dr. Pronovost’s story also highlights the need to make sure that medical residents receive adequate sleep and supervision. Dr. Pronovost made the decision to remove his patient’s breathing tube while working a 36-hour shift where he had been awake for 24 hours. Even after the 2003 reforms in working hours for residents, such working hours are still common.
In a way, the need for widespread use of checklists and the need for reduced resident hours go hand-in-hand. The medical checklist model is borrowed from the development of the aviation industry where, as planes got increasingly complicated and difficult to fly, airlines faced two choices: 1.) either train pilots for years on end (i.e., develop a more and more expert core of pilots, analogous to doctors) or 2.) replace individual autonomy of pilots with checklists. Residents are overworked because medicine has decided to give us a corps of highly trained professionals, whose autonomy is almost unbounded, and that training involves thousands of hours spent as a sleep-deprived resident.
Distracted Driving Car Accident Deaths Down In 2009
Today, the Transportation Department announced that the number of fatal car accidents caused by distracted driving declined in 2009. Nevertheless, the percentage of fatal car accidents caused by distracted driving remained steady at sixteen percent because the overall level of fatal accidents declined as well, to the lowest number since 1950.
Massachusetts Supreme Judicial Court Affirms $3.35 Million Jury Verdict For Boy Injured By Defective Escalator
 Last week, the Massachusetts Supreme Judicial Court upheld a $3.35 million jury verdict against Otis Elevator Company for an injury to a four-year old boy caused by a defective escalator that bore Otis Elevator’s name but that was in fact manufactured by an independent Chinese company, China Tianjin Otis Elevator Company, Ltd. (CTOEC). The case is an important decision that adopts part of the “apparent manufacturer” doctrine from the Restatement (Third) of Torts: Product Liability. (The Restatements are publications put out by the American Law Institute, an influential body of legal scholars; the Restatements attempt to summarize existing law and, sometimes, will suggest more progressive approaches for the law to develop.)
Last week, the Massachusetts Supreme Judicial Court upheld a $3.35 million jury verdict against Otis Elevator Company for an injury to a four-year old boy caused by a defective escalator that bore Otis Elevator’s name but that was in fact manufactured by an independent Chinese company, China Tianjin Otis Elevator Company, Ltd. (CTOEC). The case is an important decision that adopts part of the “apparent manufacturer” doctrine from the Restatement (Third) of Torts: Product Liability. (The Restatements are publications put out by the American Law Institute, an influential body of legal scholars; the Restatements attempt to summarize existing law and, sometimes, will suggest more progressive approaches for the law to develop.)
The boy was visiting his grandparents in China when his hand became trapped between the escalator skirt panel and the step tread. His hand was nearly severed mid-palm and he has suffered a permanent thirty-one percent whole-body impairment as a result.
Otis argued that it could not be held legally responsible for the defective escalator because, although the escalator bore its name and trademark, it never sold anything; it simply licensed its name and trademark to the Chinese company for the Chinese company to use in elevators it sold and provided some technical support. Otis insisted that product liability law requires it to be a seller at some point in time in order for it to be held liable for a defective product.
The Supreme Judicial Court rejected Otis’ arguments and agreed with Judge Lemire, the trial judge, who told the jury that the fact Otis need not have actually sold or manufactured the defective product in question, so long as it allowed the escalators to be sold bearing Otis’ trademark.
You can read the case here: Lou v. Otis Elevator Co.
Maybe Doctors Should Be More Like Medical Malpractice Lawyers And Work On An Outcome-Based Model
 It’s a familiar back-and-forth: doctors demonizing medical malpractice lawyers claim that they are forced to practice “defensive medicine” because of frivolous medical malpractice lawsuits; medical malpractice lawyers say that the unnecessary tests and procedures are really done because doctors make more money when they carry out more tests and procedures.
It’s a familiar back-and-forth: doctors demonizing medical malpractice lawyers claim that they are forced to practice “defensive medicine” because of frivolous medical malpractice lawsuits; medical malpractice lawyers say that the unnecessary tests and procedures are really done because doctors make more money when they carry out more tests and procedures.
This week the journal Health Affairs published the latest findings in this long-running dispute. Its conclusions? The fear of medical malpractice lawsuits adds $45.6 billion to our annual health care costs, about 2.4% of nation’s health care tab.*
But this figure is dwarfed by the costs added by the “fee-for-service reimbursement system and the incentives it provides.” In other words, if you’re looking to lower health care costs, you need to change the basis on which doctors are paid. If they are paid on a fee-for-service model, making more for every test and procedure that they perform, they will respond to those incentives by carrying out more costly tests and procedures.
If, on the other hand, they are paid on some outcome-based model (e.g., the patients in their practice lowering their weight, lowering blood pressure, etc.) we won’t have those wasteful expenditures and our health care costs will come down.
When you pay someone on a fee-for-services model, you get a lot of services and a big bill. This is becoming increasingly obvious in the legal world, where the defense lawyers work on a billable hours model. The billable hours model incentivizes lawyers to drag out a case and make everything as expensive as possible.
Ted Frank over the the tort reform website Point of Law.com had a great post on this just the other day, where he mentioned (with disgust) defense lawyers who had confided in him that they love costly drawn out litigation. (As a complete aside, Ted’s idea about recruiting defense lawyers on ideological lines is a brilliant one. Legal recruiting is expensive and inept. And for firms to keep lawyers on board, the lawyers have to enjoy or believe in what they are doing).
Personal injury plaintiff’s lawyers, on the other hand, do not work on a fee-for-service model. We work on a outcome based model: the contingency fee. We do not get paid unless we win a jury verdict or a settlement. As I’ve blogged about before, this has the effect of aligning the lawyer’s interests perfectly with the client’s.
Maybe doctors should be more like medical malpractice lawyers. It might be the number one thing we can do to lower our health care costs.
*Footnote: The study’s authors derived this number by extrapolating from a study of the costs of defensive medicine in the treatment of cardiac Medicare patients, an obviously small (and perhaps unrepresentative) group. The study did not attempt to take into account any decreases in the cost of health care brought about by any deterrent effect to medical malpractice litigation.
Don’t Drive With A Divorced Doctor In A Pick-Up Truck On Super Bowl Sunday: Some Surprising Car Accident Statistics
 My interest kindled by his blog, I’ve been reading Tom Vanderbilt’s book “Traffic: Why We Drive The Way We Do (And What It Says About Us.” It’s a fascinating quasi-anthropological study of the role of the automobile in our everyday lives. The book touches on a number of subjects, from road rage to city planning. But of greatest interest to most personal injury lawyers is his analysis of some of the surprising risk factors that play into many car accidents. Passengers would be wise to heed Vanderbilt’s advice: “Don’t drive in a pick-up truck with a beer-drinking divorced doctor on Super Bowl Sunday.”
My interest kindled by his blog, I’ve been reading Tom Vanderbilt’s book “Traffic: Why We Drive The Way We Do (And What It Says About Us.” It’s a fascinating quasi-anthropological study of the role of the automobile in our everyday lives. The book touches on a number of subjects, from road rage to city planning. But of greatest interest to most personal injury lawyers is his analysis of some of the surprising risk factors that play into many car accidents. Passengers would be wise to heed Vanderbilt’s advice: “Don’t drive in a pick-up truck with a beer-drinking divorced doctor on Super Bowl Sunday.”
Why shun doctors? They seem like a responsible lot; why are they at a greater risk of being involved in a car accident? The researchers don’t know for sure. Some possible theories include: 75 percent of doctors are male (and males are more likely to be involved in car accidents than women); doctors spend a lot of time driving in urban areas, dispensing advice via cell phone; and, last but not least, doctors may be more fatigued than the average driver (a New England Journal of Medicine study showed that interns working an extended shift are ten percent more likely to be involved in a car accident on their way home).
The Super Bowl Sunday risk factor is a famous result that was actually discovered by a doctor – Stanford researcher Donald A. Redelmeier – who was profiled in The New York Times last week for his quirky but illuminating public health research. Dr. Redelmeier’s findings that car accident fatalities spike by forty-one percent on Super Bowl Sunday prompted the National Highway Traffic Safety Administration to launch a program aimed at getting fans to stay off the road. Before the game on Super Bowl Sunday, the roads are as safe as any other time. During the game, there are actually fewer car accidents than normal because so many people are off the road, watching the game. But after the game (twenty times more beer is consumed on Super Bowl Sunday than a typical Sunday), the number of car accidents goes through the roof. Fans of the losing team – who perhaps were drowning their sorrows in alcohol (or who perhaps left the party right after the game, rather than staying to celebrate and thereby sobering up) – are much more likely to be involved in a Super Bowl Sunday car accident than fans of the winning team.
Divorce or a recent separation is linked with a fourfold increase in car crashes. The reasons for this are murky. But the research is consistent with other research showing that the never-married are much more likely to be in a car accident than the married-with-children. Having children makes you more likely to buckle up and more likely to drive cautiously (especially while the children are in the car).
Pickup trucks are another surprising car accident risk factor. More pickup truck drivers die per 100 million registered vehicles than any other style of car. Given pickup trucks’ size, you’d think that pickup truck drivers would be among the least likely to die in a car accident. But research has shown that a car’s size is of almost no importance when the car or truck collides with a fixed barrier like a tree or a bridge support. Some of the risk of pickup trucks may be connected to the fact that far more men than women drive pickups and men are much more likely to be involved in a car accident. Men also are much less likely to wear a seatbelt. Beyond those possible contributing factors, statisticians have a hard time sussing out why pickups are so dangerous.
So, whatever the reasons, don’t drive with a divorced doctor in a pick-up truck on Super Bowl Sunday.
Students Who Take Driver’s Ed More Likely To Be Involved In A Car Accident Than Those Who Do Not Take Classes?
 Lawmakers in Indiana are puzzled by a new study showing that students who take driver’s ed classes are four times more likely to be involved in a car accident than those who don’t take the classes and instead merely take the license exam.
Lawmakers in Indiana are puzzled by a new study showing that students who take driver’s ed classes are four times more likely to be involved in a car accident than those who don’t take the classes and instead merely take the license exam.
The study has led some lawmakers to propose that driver’s ed classes be overhauled. The curriculum has not been changed in 30 years.
The study seems counterintuitive but it’s easy to think of a few reasons why it might be true:
1.) The students who can afford to pay for driver’s ed classes are wealthier on average than the students who don’t take the classes and therefore are likelier to own their own car, leading them to rack up more mileage and causing them to be involved in more car accidents. The students who don’t take driver’s ed are poorer on average and therefore have less access to cars, causing them to be involved in fewer car accidents.
2.) The students who can’t afford to take driver’s ed worry that they are lesser-prepared than their driver’s ed counterparts and overcompensate by logging more hours practicing with family members or other (free) driving instructors. (This could easily be the case in a state like Massachusetts where driver’s ed only requires twelve hours of behind-the-wheel time. In Massachusetts, however, driver’s ed classes are mandatory for all drivers under eighteen.).
3.) Driver’s ed programs self-select for bad drivers: the students who enroll in driver’s ed are students who realize they need it. Driver’s ed coaches them up but doesn’t bring them to the same level as peers with better driving abilities (the least plausible explanation).
