 As today’s Globe reminds us (hat tip to Ted Frank at Point of Law for bringing the story to my attention), tonight’s blizzard will be the first large snowfall that we’ve seen since the Supreme Judicial Court abolished the so-called “natural accumulation” rule in a decision that was issued while we were enjoying the warmth of the July sun.
As today’s Globe reminds us (hat tip to Ted Frank at Point of Law for bringing the story to my attention), tonight’s blizzard will be the first large snowfall that we’ve seen since the Supreme Judicial Court abolished the so-called “natural accumulation” rule in a decision that was issued while we were enjoying the warmth of the July sun.
I’ve been meaning to blog about all the recent coverage that the case – Papadopoulos v. Target Corporation – has received in the local media. While Brian MacQuarrie’s Globe piece gets the law right, some of the coverage has bordered on the sensationalistic. For example, the other day I heard a teaser on my beloved WBUR (our local NPR affiliate) intoning that the case “eliminates virtually every excuse” that a landowner can offer to avoid liability in a slip-and-fall case involving ice and snow.
Not quite.
As I blogged in August, the case simply brings Massachusetts law into line with the common law of every other American jurisdiction by abolishing an archaic rule that lawyers called the “natural accumulation doctrine.” Prior to the Supreme Judicial Court’s decision in Papadopoulos, judicial opinions in other states referred to the natural accumulation doctrine as “the Massachusetts rule” because we were the only state to have a rule stating that property owners were not liable for injuries arising from the natural accumulation of snow and ice.
Under the new rule adopted in Papadopoulos, property owners will have a duty to use reasonable care in the removal of snow and ice from their property. That’s it. End of story. Finito. Henceforth we’ll follow the same legal rule as the other forty-nine states in our Union. That’s the big change that the local media are breathless about.
If you are the type of person who is interested in arcane developments in the law of slip-and-fall injuries in Massachusetts, you can read my original, more in-depth blog post about the changes in the law of snow-and-ice removal by clicking here.
Monthly Archives: December 2010
Medical Malpractice And Car Accidents: A Tale Of Two Public Health Problems
 In 2009, 33,963 Americans died in car accidents. 100,000 Americans are killed each year by medical errors. Given the large number of lives lost to both medical malpractice and car accidents, both qualify as important public health problems. But while we are making strides in reducing the number of lives lost in car accidents, a recent study shows the number of deaths due to medical errors has held steady over the past decade. The divergent outcomes in these two areas may be due to the different approaches we take with respect to curbing car accidents and medical malpractice deaths.
In 2009, 33,963 Americans died in car accidents. 100,000 Americans are killed each year by medical errors. Given the large number of lives lost to both medical malpractice and car accidents, both qualify as important public health problems. But while we are making strides in reducing the number of lives lost in car accidents, a recent study shows the number of deaths due to medical errors has held steady over the past decade. The divergent outcomes in these two areas may be due to the different approaches we take with respect to curbing car accidents and medical malpractice deaths.
From 2005-2008, the number of traffic deaths declined twenty-two percent. What explains this precipitous drop? As reported last week by The Wall Street Journal, researchers at the University of Michigan’s Transportation Research Institute think they have some of the answers. They chalk up the decline of car accident deaths to a combination of factors, most notably improved safety technology, more aggressive treatment of drunk drivers and stricter licensing requirements for teens.
When you look more closely at some of these factors – improved safety technology, aggressive prosecution of drunk drivers – they are largely the result of government regulation and resort to our court systems. Many car safety improvements are the result of government mandates and product liability litigation. And harsher treatment of drunk driving requires that our courts have more involvement in our lives.
While traffic deaths due to certain factors – such as distracted driving – are climbing steadily, we can see the way that society is dealing with that threat: we are passing more and more laws banning texting while driving or talking on the phone and driving. In short, when it comes to car accident deaths, we are not afraid to unleash the legal system to address problems.
But we seem to be doing the exact opposite when it comes to medical errors. We have lax regulation of medical technology, which leads to the problems you see here, here, here and here.
And instead of holding doctors legally accountable for medical malpractice, the tort reformers have us passing caps on pain-and-suffering in medical malpractice cases, caps that have virtually eliminated lawsuits against doctors in many states. Are insurance companies really going to insist that doctors implement error-avoidance technologies when the insurance have to shell out so little even in the minority of lawsuits where patients are successful?
The decline in traffic deaths that we’ve seen over the past several years is probably attributable to a lot of things – including people not being able to afford gas and therefore driving less. But the long-term graph of traffic deaths is clearly trending downward. And perhaps there’s a public health lesson in that.
DePuy A.S.R. Hip Replacement Recall Shows Flaws In FDA Approval Of Medical Implants
 As underscored by a story in today’s New York Times, the recent recall of DePuy A.S.R. artificial hips shows how a hole in the FDA’s regulatory framework for medical implants endangers millions of Americans who receive medical implants.
As underscored by a story in today’s New York Times, the recent recall of DePuy A.S.R. artificial hips shows how a hole in the FDA’s regulatory framework for medical implants endangers millions of Americans who receive medical implants.
DePuy A.S.R. artificial hips were touted as next generation of artificial hips – a new technology that would allow for hip replacement surgeries involving the removal of less of a patient’s thigh bone. The A.S.R. or Articular Surface Replacement technology, it was thought, would resurface portions of bone that were removed in conventional hip replacements. DePuy, a Johnson & Johnson subsidiary, also promoted the A.S.R. technology as likely to last longer than rival hip replacements – predicting a product lifetime of 15 years or more.
What steps did DePuy have to go through to bring the A.S.R. artificial hips to market? Were there years and millions of dollars spent double-blind randomized clinical trials before the FDA finally approved the DePuy ASR? No. In fact, because FDA regulations allow medical implants to be sold without clinical testing if they resemble devices already approved for use in patients, the DePuy ASR made it to market without clinical trials.
DePuy claimed the A.S.R. resembled another hip prosthesis that it had already brought to market called the Ultima. The Ultima, however, had a completely different cup design than the ASR. Despite the dissimilarities between the A.S.R. and the Ultima, the FDA regulations allowed the A.S.R. to be sold without testing.
Because of the absence of any clinical testing of the DePuy ASR, orthopedic surgeons who were implanting the ASRs had no data to go on about the ASR’s effectiveness. All they had were DePuy’s very compelling promotional materials – their advertising – which seemed to demonstrate that the ASRs were much more durable and longer-lasting than conventional hip replacements.
When the DePuy ASRs began being implanted in patients, problems almost immediately began cropping up. The grinding on metal-on-metal parts within the ASR released cobalt ions that killed tissue, causing pain and, in some cases, permanent disability.
But doctors had no idea how widespread the problems were with DePuy ASR artificial hips because FDA regulations do not require reports of problems relating to this type of implant to be maintained in any sort of central database. Orthopedic surgeons who reported problems with the A.S.R. to DePuy were told that the problem lay with their surgical technique and not with the implant.
As a result of the mounting complaints about the ASR, DePuy reportedly knew of its defects as early as 2008. However, DePuy did not recall the XL Acetabular Head System until late August of this year.
There are basically two frameworks for addressing the safety of medical devices. One is regulatory: government agencies insist on certain testing and safety precautions before a product can be brought to market. The other lies in tort: people injured by devices like the DePuy ASR hire trial lawyers to sue for their injuries. We’ve blogged before about how famous economists like Milton Friedman have favored robust tort remedies in protecting consumers. But it seems that increasingly we are moving to a regime that favors regulatory protections over tort rights.
Thankfully, those who were injured by DePuy ASR hip prostheses still have the right to hire lawyers to bring suit for the injuries they’ve suffered. If it were up to some people, however, injury lawyers would not be protecting the DePuy ASR victims, only a hollow patchwork of regulatory protections would be.
Why You Should Steer Clear Of A “Settlement Mill” If You Have A Serious Car Accident Case And Tips On How To Spot One
 A recent article by law professor Nora Freeman Engstrom in the Georgetown Journal of Legal Ethics explains why personal injury “settlement mills” exist and why, if you have a serious personal injury case, you should make sure that your lawyer is not running a settlement mill (hat tip Point of Law and Drug and Device Law for the original post).
A recent article by law professor Nora Freeman Engstrom in the Georgetown Journal of Legal Ethics explains why personal injury “settlement mills” exist and why, if you have a serious personal injury case, you should make sure that your lawyer is not running a settlement mill (hat tip Point of Law and Drug and Device Law for the original post).
A “settlement mill” is a law firm that handles a high volume of cases, usually specializing exclusively in a certain niche like car accident cases. These law firms, relying mainly on paralegals and administrative assistants, settle an astounding number of cases. In short, they focus on quantity and not quality. They aren’t interested in trying cases because, with the volume of cases that they have, there’s just no time for jury trials.
Why do these settlement mills exist? Prof. Engstrom theorizes that it’s because the insurance companies actually like settlement mills, despite having to fork over money to them in settlements. Professor Engstrom writes that insurance companies and settlement mills “share two sets of overlapping interests: speed and certainty.” Both insurers and settlement mill lawyers want to close out cases quickly – the insurers to take the case off their books and the lawyers so that they get paid.
The desire for certainty that insurers and settlement mills share comes in the form of certainty about damages. An insurance company doesn’t want a case to get to jury trial where a jury can award virtually any amount in damages for pain-and-suffering; it wants the certainty of a pre-trial settlement that caps its liability. Likewise, the lawyers at settlement mills want the certainty of a settlement rather than rolling the dice in a trial they’ll spend hundreds of hours preparing for but might ultimately lose.
As a result of their overlapping interests, settlement mills and insurance companies work out a tacit bargain: the insurance companies pay out small settlements of say $2,500-$5,000 to the settlement mills even in questionable cases. What they get in exchange is the certainty that the serious case, the one that might be worth millions in front of a jury, will almost assuredly never get to trial.
How can you tell if your lawyer is running a car accident settlement mill? Engstrom’s article identifies a number of characteristics of settlement mills, but they’re often hard for an outsider, such as a client, to assess. One red flag that she does mention is a so-called tiered contingency agreement. Under a tiered contingency agreement, the fee that you pay your lawyer goes up if your lawyer has to take the case to trial. If your lawyer offers you a tiered contingency agreement, run, don’t walk, away.
In addition to Engstrom’s warning about tiered contingency fee agreements, I’ve come up with a few more tips about how to spot a settlement mill:
- The law firm is very neat and organized. This one may sound a little funny. Don’t you want a lawyer who’s organized? Well, you want a lawyer who’s on the ball, but that doesn’t necessarily go hand in hand with having an office that’s immaculate at all times. But settlement mills are. They have to be ultra-efficient to handle the volume of cases that they do. That means they have to have an incredibly organized office. From the outside, it looks like they’re running a tight ship but all it really means is that they’re interested in turning over your case and moving on to the next one.
- They use a lot of specialized software. Companies come to me all the time trying to sell me legal software. I never buy any of it because I have no interest in buying and learning a piece of software that will save me a few seconds a day. Plus, most of what I do is too diverse for specialized software to be of much use to me. But in law offices that focus on a high volume of the same kind of cases, proprietary software is a necessary time-saver. So, for example, most title attorneys who do a great deal of residential closings have software programs that do a lot of the work for them. So too a lot of personal bankruptcy lawyers. The same holds true for the auto accident settlement mill lawyer.
- If you get to talk to a lawyer, the lawyer always calls you back instead of immediately taking your call. At a settlement mill, a paralegal or administrative assistant is doing most of the work on your case. And the settlement lawyer has way too many cases to have time to personally take your phone call. So it will be virtually impossible to get your lawyer on the phone. But for me, the dead giveaway is when you finally get to the end of your rope and go ballistic on the lawyer’s secretary, forcing her to talk to you on the telephone. You won’t be patched through by the secretary directly to the lawyer; the lawyer has so many clients that she knows nothing about you or your case and has to refresh her memory with the case file before calling you back to speak to you.
Medicare’s Dialysis Program: An Illustration Of Why US Health Care Costs Are So High
 Over the past month an article written by Robin Fields and originally printed in Pro Publica has attracted a great deal of attention and earned a reprint in The Atlantic. The article, about Medicare’s dialysis benefit, illustrates the problems at the heart of much of American health care.
Over the past month an article written by Robin Fields and originally printed in Pro Publica has attracted a great deal of attention and earned a reprint in The Atlantic. The article, about Medicare’s dialysis benefit, illustrates the problems at the heart of much of American health care.
In 1973, faced with the specter of the wealthy receiving life-saving dialysis while stingy insurance companies denied coverage to the poor, Congress passed a law amending the Social Security Act so that every patient in need of dialysis treatment would receive it. Nearly four decades later, this once-obscure program has ballooned, gobbling up nearly six percent of Medicare’s budget.
Today, Medicare spends $77,000 a year on each dialysis patient (most likely the highest rate in the world) and the US has the world’s highest fatality rate for dialysis patients. The story of how this came to pass illustrates a lot of the problems with US health care.
As Fields’ article makes clear, people respond to incentives. When the system compensates health care providers for each procedure performed – as the US health care system’s fee-for-service model generally does – you get a lot of treatment procedures done, at a high pricetag. Since its inception, Medicare’s dialysis program has paid treatment centers a flat fee for each patient treated without regard to the efficacy of treatment or health outcomes.
Thus, Medicare’s dialysis program produced a burgeoning number of clinics where people could receive treatment, but the treatment is, judged by worldwide health care standards, subpar. A higher percentage of Americans in dialysis treatment die than in any developed country. Fee-for-service means that treatment centers are just interested in completing and billing out procedures, even if their substandard treatment ultimately kills the patient who lays the golden egg.
A fee-for-service model also means that any outcome that does not get compensated falls by the wayside. Because treatment centers are paid for how many patients they treat and not for how healthy they keep the patients, it’s not uncommon for the the clinics to be dirty and infection-prone, their walls smeared with contaminated blood.
Because American health care professionals are mostly compensated on a fee-for-service basis (unlike in much of the rest of the world), American dialysis patients are more likely to suffer from complicating factors like diabetes and hypertension than patients elsewhere. The typical American doctor has no financial incentive for preventing his patients from developing Type II diabetes or hypertension, or for controlling those conditions. The typical American doctor is compensated only for seeing and treating those patients, so our dialysis patients are also less healthy than in the rest of the world.
Fee-for-service health care, as we have in the US, also dooms price controls to failure. As the price of dialysis machines fell, treatment centers were making money hand-over-fist as the treatment was less expensive to provide while the reimbursement rates remained high. Medicare realizing it could cute reimbursement rates, while still enabling operators to make a profit, did just that.
What happened? The use of certain expensive injectable drugs, such as Epogen – that are used to treat side effects – skyrocketed. Medicare was continuing to provide generous reimbursement rates for these injectable drugs so patients who did not need these drugs got them. Italy, which has the lowest dialysis mortality rate in the world, gives Epogen to half as many of its dialysis patients. Today, doses of Epogen are Medicare’s single highest pharmaceutical expenditure.
The US badly needs to move away from the fee-for-service model toward a model that provides incentives for high-quality, low cost care. The same Health Affairs study from a couple months ago that pegged the direct and indirect costs of medical malpractice lawsuits at two percent of our heath care spending, said that the cost of medical errors was dwarved by the costs added by fee-for-service.
The good news is that next year Medicare is rolling out a new reimbursement system. Treatment centers will no longer be able to bill separately for injectables. And we’ll see the debut of at least one outcome-based (rather than fee-based) metric: clinics could lose as much as two percent of their Medicare funding if they fail to meet certain minimal thresholds for anemia-management and dialysis-adequacy, as measured by patient blood tests.
It’s a modest start, but it’s a step in the right direction. And, in the meantime, let’s stop acting like American health care is going bankrupt compensating those who have been maimed and killed by medical errors.
ECRI Institute Releases List Of Top Ten Threats To Patient Safety
 Last week we blogged about a new study published in The New England Journal of Medicine showing that patient safety has not improved in the ten years since the Institute of Medicine published its famous study showing that medical errors kill 98,000 Americans a year.
Last week we blogged about a new study published in The New England Journal of Medicine showing that patient safety has not improved in the ten years since the Institute of Medicine published its famous study showing that medical errors kill 98,000 Americans a year.
How to improve patient safey? This week the ECRI Institute released its fourth annual Top Ten list of threats to patient safety. They are:
1. Radiation Overdoses: A subject we’ve blogged about here, here and here.
2. Alarm Hazards: Whenever you go to a hospital, you hear dozens of alarms buzzing, alerting staff to problems with patients. The danger comes when nurses or doctors silence the alarms to stop the annoying ringing, or simply ignore them.
3. Cross-contamination from flexible endoscopes: Most infection problems are preventable, if attention is paid to them.
4. Radiation overdoses in CT scans: Again a subject we’ve blogged. See above.
5. Problems with medical records: Information Technology needs to improve so that patient records are more easily obtained and health care providers are working on interoperable systems.
6. Luer Connections: Luer Connections are important parts that hook up needles, catheters and tubes. When improperly connected, they can introduce improper gases or liquids into a patient’s bloodstream.
7. Overdosage through PCA infusion pumps: PCA pumps administer set doses painkillers. When misprogrammed, they can overdose a patient.
8. Needle sticks: They’re a problem that affects not only health care providers but also patients.
9. Surgical fires: Surgical fires are as common as wrong-site surgeries. In this week’s news was a gruesome case where a patient’s throat was set on fire during laser surgery.
10. Defibrillator problems: This problem of increasing urgency was added to the list this year.
Link Roundup
- A new NHTSA study reveals that, as police drug test increasing numbers of drivers in fatal accidents, the number of drivers found to be intoxicated is increasing. Right now, nearly two-thirds of drivers involved in fatal accidents are drug tested and eighteen percent of those test positive. One-third of drivers killed in fatal car accidents have drugs in their system.
- A really amazing graphic showing how different countries’ spending on health care has increased from 1960-2008 as a percentage of their GDP:
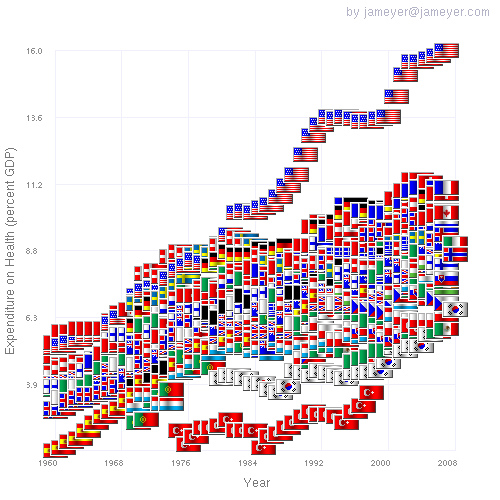
(Hat tip to the creator of this graphic). You can’t blame that uptick on the medical malpractice lawyers.
- A new Vanity Fair article takes a hard look at a topic we’ve examined before: the outsourcing of clinical trials to countries in the developing world. (Hat tip Prof. Bernabe, who has been blogging this topic for some time).
