 So, following up on my blog post of a couple weeks ago, I finally got a chance to read “Poisoned: The True Story Of The E. Coli Outbreak That Changed The Way Americans Eat” by Jeff Benedict. “Poisoned” tells the story of Bill Marler’s lawsuits against Jack-in-the-Box for the 1993 E. Coli O157:H7 outbreaks at its restaurants.
So, following up on my blog post of a couple weeks ago, I finally got a chance to read “Poisoned: The True Story Of The E. Coli Outbreak That Changed The Way Americans Eat” by Jeff Benedict. “Poisoned” tells the story of Bill Marler’s lawsuits against Jack-in-the-Box for the 1993 E. Coli O157:H7 outbreaks at its restaurants.
I was excited to read the book because, based on the review that I read in The New York Times, I expected the story to be a real-life David v. Goliath legal thriller in the mold of Jonathan Harr’s “A Civil Action” (the book about the legendary Woburn, MA toxic tort case that was made into a motion picture starring John Travolta).
Sadly, “Poisoned” is not much of a legal thriller. Nor does it really touch upon much of the technology/science behind food safety and the way that Marler’s litigation changed food safety protocols. I was hoping the book would deliver on one of those fronts – either as a legal thriller or, as its subtitle suggests, a story about the technical side of food safety.
Category Archives: Foodborne Illness
Book Review Of “Poisoned: The True Story Of The E. Coli Outbreak That Changed The Way Americans Eat”
 I’ve been wanting to read Jeff Benedict’s “Poisoned: The True Story of the Deadly E. Coli Outbreak That Changed The Way Americans Eat,” since I heard Benedict interviewed on this RadioBoston episode on the E. Coli outbreak in Germany.
I’ve been wanting to read Jeff Benedict’s “Poisoned: The True Story of the Deadly E. Coli Outbreak That Changed The Way Americans Eat,” since I heard Benedict interviewed on this RadioBoston episode on the E. Coli outbreak in Germany.
Monday’s New York Times carried a review of “Poisoned” by Dr. Abigail Zuber that got me truly amped up to read a copy. From hearing Benedict interviewed, I labored under the misimpression that “Poisoned” was a book about public health, about the food industry and the science of food poisoning.
As Zuber’s review highlights, however, “Poisoned” is actually a real life legal thriller in the mold of Jonathan Harr’s “A Civil Action.”
“Poisoned” focuses on the infamous Jack-in-the-Box E. Coli O157:H7 outbreak that killed four children and injured hundred of others in Western states in 1993.
As Zuber writes, the Jack-in-the-Box outbreak led to a “David and Goliath” battle between Jack-in-the-Box and the poisoned customers. The legal struggle pitted Bill Marler (then, according to Zuber, “a financially struggling young lawyer who, through a series of happenstances came to represent Seattle’s most damaged victim”) against Bill Piper, an “established Seattle lawyer,” who wore suspenders with pictures of nude women on them (!) and who was known to be “devastatingly effective in court.”
You may already know the post-script: Marler won a $15.6 million dollar jury verdict on behalf of client and the entire food service industry overhauled its food-preparation protocols.
I just went to Amazon.com and ordered my own copy of “Poisoned.” I hope to have my own review soon.
Europe’s E. Coli O104:H4 Outbreak: Facts And Lessons
 Although the story’s been in the news for nearly two weeks, I’ve hesitated blogging about the outbreak of E. Coli O104:H4 contamination in Europe because it seemed like every time I turned around, there was some new update rendering the previous theories and hypotheses null and void.
Although the story’s been in the news for nearly two weeks, I’ve hesitated blogging about the outbreak of E. Coli O104:H4 contamination in Europe because it seemed like every time I turned around, there was some new update rendering the previous theories and hypotheses null and void.
At this point, it seems that this much is clear. According to the latest Bloomberg report, tainted food products carrying the O104:H4 bacteria have caused at least 23 deaths in Europe and poisoned 2,429 others, 674 of them seriously.
The “index” (earliest) cases of the outbreak occurred around May 2, but it was not until May 22 that public health authorities acknowledged that we had had a full-fledged outbreak on our hands.
Although initially it was suspected that cucumbers might be the source of the outbreak and, later, it was thought to be bean sprouts, experts from the World Health Organization insist that we don’t know the vector of the contamination and might never know.
“If we don’t know the culprit in a week’s time, we may never know,” says Dr. Guenael Rodier of the WHO. According to Dr. Rodier, the food products that caused the outbreak have likely disappeared from store shelves, making it harder to link patients with the source or sources of the contaminated food.
The Centers for Disease Control reports four Americans have been sickened by E. coli O104:H4 within the past several weeks, all of whom had recently traveled to Germany and all of whom are believed to have suffered the food poisoning there. The CDC have issued a travel warning to Americans traveling to Germany.
The E. Coli O104:H4 strain that is ravaging Germany is not the same strain of E. Coli that has hurt so many American consumers. The strain of E. Coli food poisoning that first popped into American consciousness with the Jack-in-the-Box epidemic in 1993 and that continues to be a recurring problem in the American food supply chain is E. Coli O157:H7. The two different strains, however, are both capable of causing massive kidney failure leading to death or permanent disability.
We’ve talked a lot on this blog about two different approaches to protecting consumers from injury: government regulation and private tort lawsuits. We’ve discussed one problem with relying on government regulation to protect us – that regulatory bodies are susceptible to “regulatory capture” by the special interests they are supposed to regulate.
It seems the regulatory approach is especially inadequate within the European Union, where competing national interests and cross-border limitations on investigators may make it difficult to combat outbreaks such as the present one. As one American public health official, Dr. Michael Osterholm, has said, “If you gave us [American public health officials] 200 cases [of E. coli poisoning] and five days, we would be able to solve this outbreak.” Osterholm went on to describe the European effort as “erratic” and a “disaster,” saying that German officials should have done more to interview patients in the early days of the outbreak. Instead, German officials leveled an accusing finger first at the Spanish, then at the French.
Given the way the Germans have handled this outbreak, you have to wonder whether it’s simply incompetence or whether there are political forces at play that have hindered the investigation.
At any rate, let’s hope that public health officials manage to track down the source of the E. Coli O104:H4 outbreak and that E. Coli O104:H4 does not make its way into the American food supply.
Link Roundup
- A new NHTSA study reveals that, as police drug test increasing numbers of drivers in fatal accidents, the number of drivers found to be intoxicated is increasing. Right now, nearly two-thirds of drivers involved in fatal accidents are drug tested and eighteen percent of those test positive. One-third of drivers killed in fatal car accidents have drugs in their system.
- A really amazing graphic showing how different countries’ spending on health care has increased from 1960-2008 as a percentage of their GDP:
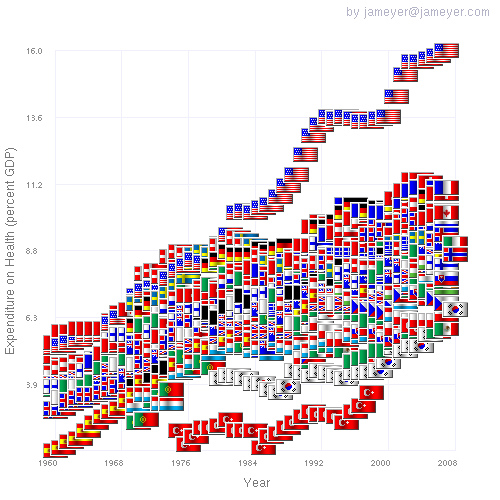
(Hat tip to the creator of this graphic). You can’t blame that uptick on the medical malpractice lawyers.
- A new Vanity Fair article takes a hard look at a topic we’ve examined before: the outsourcing of clinical trials to countries in the developing world. (Hat tip Prof. Bernabe, who has been blogging this topic for some time).
Putting All Of Your Eggs In The Same Basket: The Story Of The Salmonella Egg Recall
 Unless you’ve been living under a rock, you couldn’t have missed the past week’s nationwide recall of a half-billion eggs feared to be contaminated with salmonella bacteria. How could half a billion eggs – more eggs than there are people in the United States – become unsalable?
Unless you’ve been living under a rock, you couldn’t have missed the past week’s nationwide recall of a half-billion eggs feared to be contaminated with salmonella bacteria. How could half a billion eggs – more eggs than there are people in the United States – become unsalable?
Part of the story is that we’ve been putting all of our eggs in the same basket. All of the recalled eggs originate with two producers in Iowa – Wright County Egg and Hillendale Farm. Iowa has come to dominate egg production nationally because the cost of feed grain is so cheap in Iowa, because of Iowa’s abundant corn fields. Although the cost of feed grain in Iowa is probably only marginally cheaper than elsewhere in the country, the huge scale of modern agribusiness means that egg production will be located in a few centralized locations in Iowa.
In short, we put all of our eggs in a few Iowa-based egg baskets. This means when there is a problem in the supply chain, it will have massive implications. These Iowa plants with their Concentrated Animal Feeding Operations (CAFOs) are the ideal breeding grounds for the spread of any disease or contaminants: you have massive, very dense populations whose members, once infected, travel across all fifty states.
Also, with that many egg-laying chickens in such close proximity, prophylactic antibiotics are the order of the day to prevent epidemics that would kill off the chickens laying the golden eggs. But regimens of prophylactic antibiotics of course have side effects: they build up resistance and cause new strains of bacteria to evolve.
What’s the solution? Critics of a pending food safety bill (previously blogged about here), including Walter Olson of the Cato Institute, insist that more regulation is not the answer – that the cost of complying with new regulations will crowd out small-scale producers, such as organic and free range egg producers. You can read Olson’s critique here, in part of a New York Times symposium on the salmonella egg recall.
Of course, as many have rightfully pointed out, the blame for the salmonella outbreak lies not only with the degree of regulatory oversight but with the framework of the oversight. Two different government agencies are responsible for the safety of two intricately connected foodstuffs: the chicken and the egg. The Food and Drug Administration is responsible for egg safety while the Department of Agriculture regulates chickens. (The same bizarre regulatory framework applies to cows and their milk). Having one government agency that oversees both chickens and their eggs might be more efficient. Of course that’s almost too much to hope for.
Critics of new regulation, like Olson, also maintain that big time egg producers like Wright Egg and Hillendale farm already have market incentives to get uncontaminated food to market. Having to destroy half a billion eggs is going to cost them and their shareholders dearly. Yet such a claim would seem to be belied by the checkered safety records of both Wright County Egg and Hillandale Farms. In 2000, the owner of Wright County Egg was cited as a “habitual violater” of Iowa environmental law. A few years before that, the egg supplier paid $2 million dollars in fines for safety violations at a Maine farm. Economies of scale can apply not only to production, but also to avoiding regulation. A small time farmer skips a safety precaution and profits a little by it, but when a large agribusiness cuts the same corner it reaps much larger savings.
Massive Iowa egg producers are probably here to stay. Americans, and people around the world, demand low-cost food. So what should we be doing? Well, the FDA’s new egg safety regulations that went into effect in July will help prevent another salmonella egg recall of this scale. Additionally, a salmonella vaccine that is given to hens in Britain and New Zealand has proved effective there.
But, more than likely, we’re going to see more outbreaks on even bigger scales as agribusinesses try to squeeze more productivity out of every square foot of their operations.
E. Coli Poisoning: Pulitzer Prizes, CDC Reports And New Legislation
A little over a week ago, the CDC announced that 2009 saw a decline in reported cases of E. coli O157 poisoning. E. coli O157:H7 is one of the strains of E. coli that is most toxic to humans and can cause one of the severest forms of food poisoning.
Lest the news lead us to become complacent about food safety, the CDC’s announcement essentially coincided with the announcement of the Pulitzer Prize committee that Michael Moss, a New York Times reporter, was awarded a Pulitzer for his investigative work in a story about the E. coli poisoning of Stephanie Smith, a 22-year old woman who became infected with E. coli through a hamburger patty.
The E. coli infection left Stephanie brain injured, unable to walk and with a serious kidney condition called Hemolytic Uremic Syndrome, that will necessitate multiple kidney transplants over the course of Stephanie’s life.
If you think our government should be doing more to prevent tainted food, like the E. coli that poisoned Stephanie Smith, from making its way to our plates, there’s good news for you: a bill, S. 510: FDA Food Safety Modernization Act, is currently pending in the Senate that would require more stringent food inspections. If you’re a Massachusetts resident, call Senators Kerry and Brown and let them know you’re in favor of safer food.
The FDA Has No Regulations About Acceptable Bacterial Levels In Bagged Salads: Sign Petition To Get Them
Umm, is it 1906 again? Do we need another Pure Food and Drug Act?
Last month, Consumer Reports ran an article entitled Bagged Salad: How Clean?, revealing that some bagged salads contain disturbingly high levels of bacteria and highlighting that there are no FDA regulations about acceptable bacterial levels in leafy greens.
Now the FDA has opened a special docket, where you can register your vote supporting food standards for leafy greens and urging “zero tolerance” for bacteria like E. Coli O157:H7, salmonella and listeria, a standard that already exists for other food products.
FDA Issues Warning To Kellogg Over Listeria Bacteria At Eggo Plant
The consumer protection blog, WalletPop, reports on the Food and Drug Administration’s warning to an Eggo waffle plant about listeria bacteria contamination.
This is not the first problem that Eggo has had with listeria. Last summer, Eggo had to recall buttermilk waffles that were manufactured at the same plant because of fears of listeria contamination.
Consuming food contaminated with listeria bacteria can lead to serious illness or even death. One University of Florida study estimates that the mortality rate of those infected with listeria is about twenty-five percent.
Are You Risking Food Poisoning By Ignoring Expiration Dates?
In today’s Slate is an article by Nadia Arumugam titled: “Ignore Expiration Dates: ‘Best by,’ ‘Sell by,’ and all those other labels mean very little.” While I might disagree with her about how tasty expired food is, the last paragraph of the article contains a lot of wisdom when it comes to freshness labels and food safety:
“Expiration dates are intended to inspire confidence, but they only invest us with a false sense of security. The reality is that the onus lies with consumers to judge and maintain the freshness and edibility of their food–by checking for offensive slime, rank smells, and off colors. Perhaps, then, we should do away with dates altogether and have packages equipped with more instructive guidance on properly storing foods, and on detecting spoilage. Better yet, we should focus our efforts on what really matters to our health–not spoilage bacteria, which are fairly docile, but their malevolent counterparts: disease-causing pathogens like salmonella and Listeria, which infect the food we eat not because it’s old but as a result of unsanitary conditions at factories or elsewhere along the supply chain. A new system that could somehow prevent the next E. coli outbreak would be far more useful to consumers than a fairly arbitrary set of labels that merely (try to) guarantee taste.”
It’s true: while improper food preparation at home or in a restaurant can cause food poisoning, the most virulent forms of food poisoning are caused neither by domestic food preparation or food that has spoiled – the worst forms of food poisoning originate at the factories. If a product is OK when it makes it to your grocer’s shelf, it probably won’t do much harm to you, even if you consume it past a “sell by” date. But if a product has a problem before it reaches your grocer’s shelf, you’re probably facing a serious case of food poisoning.
More Than A Dozen Massachusetts Consumers Suffer Salmonella Poisoning In Outbreak
Recently, the United States Department of Agriculture instituted the recall of 1,240,000 pounds of Italian sausage manufactured by Rhode Island-based meat packing company, Daniele International, after discovering that a sample of their black pepper salami contained salmonella.
On Wednesday, the Centers for Disease Control announced that, between July 2009 and the present, approximately 225 people in 44 states have been infected with a particular strain of salmonella, Salmonella Montevideo. Thirteen Massachusetts consumers have been infected with Salmonella Montevideo during that time. Some people believe that at least some of the Salmonella Montevideo episodes can be linked to Daniele International’s black pepper sausage.
Here is a CDC map of the outbreak:
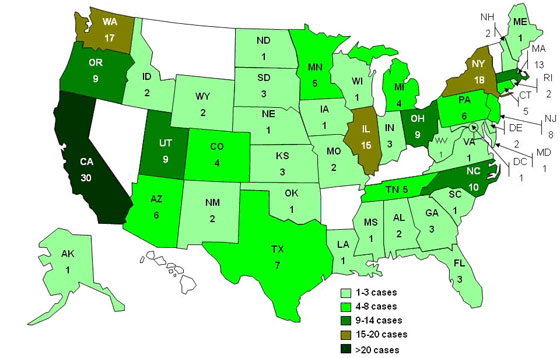
Today, the Associated Press reports that a Chicago man, who suffered salmonella poisoning, has filed a lawsuit against Daniele International and two of Daniele’s pepper suppliers, saying that they failed to take steps to prevent the outbreak.
Salmonellosis, the type of food poisoning caused by consuming salmonella-tainted food, typically produces symptoms such as fever, nausea and cramping. However, in children, the elderly and those with weakened immune systems, salmonellosis can be fatal.
We will keep you updated on this recall and further lawsuits against Daniele International.
